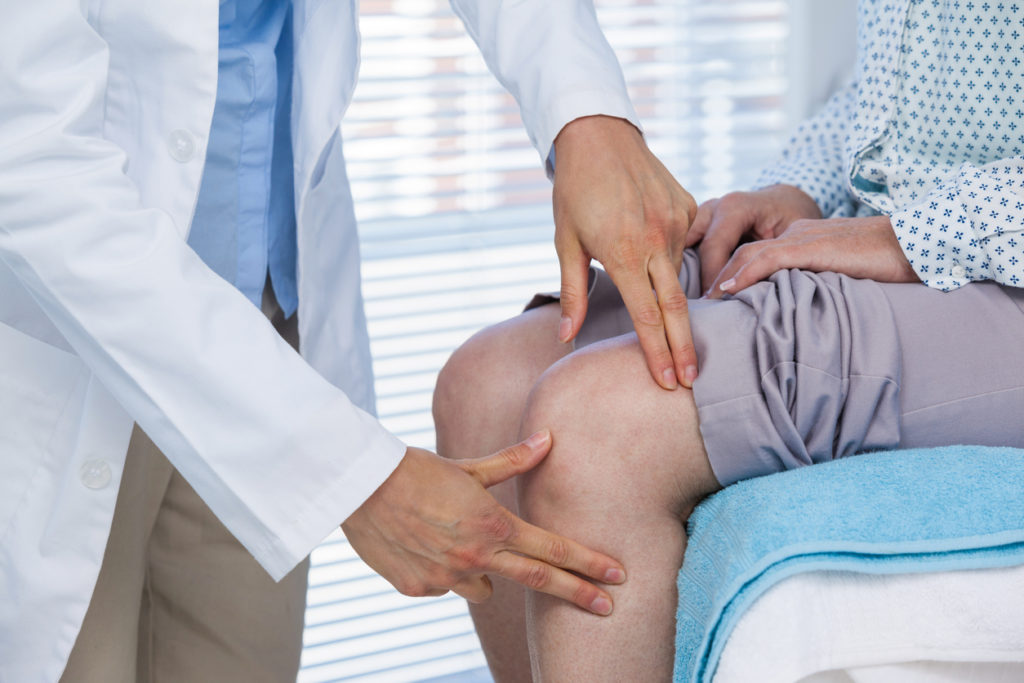
What Causes Fibromyalgia Flare Ups And How Can They Be Prevented?

Many adults suffer from fibromyalgia, and there are still many questions surrounding this diagnosis. Today, we’ll go over one of the most common questions: what causes fibromyalgia flare ups and how can they be prevented?
Fibromyalgia affects about 10 million Americans. That means millions of people are struggling to cope with pain that doesn’t have a diagnosable origin. According to the Center for Disease Control, fibromyalgia can cause:
- Pain all over the body
- Fatigue
- Sleep disorders
- Depression
- Anxiety
- Memory problems
- Headaches, and more
The word “chronic” is a significant part of defining fibromyalgia. Your negative systems have persisted for months or longer. The hardest thing to accept about fibromyalgia is not being able to determine an exact cause.
What Causes Fibromyalgia?
The exact cause of fibromyalgia has yet to be discovered. It may vary from person to person. However, many researchers believe the central nervous system, or a defect in the central nervous system, is thought to play a major role. To diagnosis fibromyalgia, it’s not as simple as taking a blood test or imaging results. Instead, your pain management specialist will perform a lengthy evaluation to include family medical history, personal history, physical exam, and testing in the body’s tender points to check for arthritis or other reasons for inflammation and pain.
For many, getting a diagnosis of fibromyalgia may mean your family doctor uses the process of elimination or figuring out what your problem is not. Thus, it is imperative to request an assessment with a pain management specialist, not your family doctor, as soon as possible.
If you have fibromyalgia, then you know the negative symptoms all too well. You may also know what is meant by fibromyalgia flare ups.
What Are Fibromyalgia Flare Ups?
Having fibromyalgia means you experience some negative symptoms regularly. Some days you can function and notice a few signs. Other days you can’t get out of bed without excruciating pain. When your negative symptoms increase in intensity, this is referred to as a flare up. Fibromyalgia flare ups will range in intensity and length of time you experience them. Some people may have flare ups for a few hours; some may have them for a few days.
The number one noted cause of flare-ups is stress or feeling like you are under a lot of pressure because stress leads to so many other health issues that also contribute to flare ups.
For example, when you feel stressed, you aren’t able to get a good night’s sleep, your digestive system may be disturbed, which will affect your diet and nutrition. All three cause fibromyalgia flare ups on their own. Together, they are like a tornado working its way through your body.
Common Fibro Flare Up Symptoms
The most reported symptoms associated with fibromyalgia flare ups include feeling pain throughout the body. This pain can occur in the joints, muscles, bones, or all of the above. The location is not as important as is the fact that it is widespread.
Other symptoms include:
- Feeling so tired it is hard to get out of bed or accomplish ordinary daily routines
- Trouble remembering what should be simple things- your memory feels foggy- often called “fibro fog”
- Any kind of problems related to sleep
- Feelings of sadness or anxiety for no apparent reason
- Stiffness, especially after being inactive for a while
What Causes Fibromyalgia Flare Ups?
As mentioned before, physiological or psychological stress is one of the biggest causes for fibromyalgia flare ups. It is not the only reason, however.
Change is another major factor triggering flare ups. This may be because changes can be stressful. If you are experiencing a flare up for what seems like no reason, consider possible changes that have happened recently. Changes in your schedule, diet, sleep patterns, treatment, and even the weather can lead to a fibromyalgia flare up. Something else that changes are your hormones. In both men and women, hormonal changes happen.
You must have your hormonal balance evaluated by a pain management specialist. They have simple fixes to rebalance your hormones if needed. Also, menstrual cycles of women are directly related to flare ups, likely because of hormone fluctuation and changes within the body. Do you know how your flare ups always seem to happen just before the family reunion or the annual Christmas party? Well, significant events are often a reason fibromyalgia symptoms increase in intensity.
Other triggers can include traumas to the body like an injury, operations, or even getting a tattoo.
Treating Fibro Flare Ups
Prevention is always the best solution. Having said that, preventing all flare ups related to fibromyalgia is impossible. But if there is something you can do to get rid of some, it’s worth the effort. There are even things you can do to reduce the intensity of pain you feel when you can’t prevent a flare up.
Implement sleep hygiene or a nightly routine that helps you fall asleep, stay asleep, and wake up feeling restored and rested. If you have a sleep disorder, work with a pain management specialist to resolve the problem.
Practice stress management daily. Activities for stress management don’t have to be long or overwhelming. Create a plan with your pain management team. Start practicing deep breathing, yoga, or meditation for ten minutes, and increase the amount over time. I know it’s hard, especially during these Coronavirus times, to avoid negative news. However, engaging in all the adverse news reports will only lead to more significant stress and a higher potential for a flare.
Create a healthy diet plan that reduces your intake of processed sugar, which has been proven to increase inflammation in the body. Other treatments that help include staying active as much as possible. Being inactive will lead to stiffness and more pain. Attending physical therapy is a great way to remain active without overdoing it. Join a support group with others who have fibromyalgia.
Your pain management specialist can provide nerve stimulation therapies to help ease fibromyalgia flare ups by interrupting the pain signals sent to your brain. Finally, create an emergency flare up kit, your go-to bag of tricks that you have found to help you during previous flare ups.
You can manage fibro flare-ups. Work with your pain management team to create your plan today.
Pain Assessment: How Bad is Your Pain?

Science argues that pain is a subjective experience. Some pain experts agree that part of feeling the pain is how your brain is interpreting it. Fortunately, whether it’s all in your head or not, there are pain assessment tools to determine how bad your pain is. Here are different types of assessment tools to help you accurately portray your pain levels to professionals.
The 10-Point Pain Scale
Many doctors use a 10-point pain assessment scale, with 0 being no pain and 10 being an excruciating, debilitating pain. Yet, even this can be highly subjective. Two people with the same degree of pain might assess their pain differently – one at a level 5 and the other at a level 7 – depending upon their relative experiences. Because of this, there are other pain assessment tools to consider as well.
Other Pain Assessment Tools
To help people be more specific about their pain assessment and to determine just how severe pain might be, the LOCATES scale can help draw more information about the type of pain a person is experiencing. The LOCATES scale was developed by the American Pain Foundation (no longer in operation), and it continues to be a reliable tool to facilitate communication between health professionals and their patients.
The LOCATES pain assessment scale asks for the following information:
L – Location of the pain: Where is your pain and does it travels to other parts of your body?
O – Other associated symptoms: Do you have nausea, numbness, or weakness with your pain?
C – Character of the pain: Is it throbbing, sharp, dull, or burning?
A – Aggravating and alleviating factors: What makes the pain better or worse?
T – Timing of the pain: How long does the pain last? Is it constant or intermittent?
E – Environment: Where do you experience the pain most often – for example, while working or at home?
S – Severity of the pain: How would you rate your pain on a 0-to-10 pain scale, from no pain to worst ever?
While the above tool does use a 10-point pain assessment scale, it also invites more details about the level, type, factors, and symptoms of the pain. Those experiencing pain may want to share their answers to the above questions with their healthcare provider. Conveying these answers to your doctor can help you both create a pain management plan.
The Process of Pain
The process of pain is actually somewhat complex. It begins with the body’s vast neural network and millions of tiny sensors that exist throughout the body. Pain can be experienced when a nerve in the body has been triggered. However, there must be a certain amount of stimulus for pain to trigger.
For example, let’s say you have a bowling ball resting on your big toe. Yes, it’s heavy and it’s likely uncomfortable, but the weight of the ball isn’t enough to stimulate pain. Yet, if a bowling ball were to drop on your big toe from a few inches up, the falling weight of the bowling ball would stimulate a great deal of sensors, activating a nerve. This nerve, in turn, will produce a signal that travels up the spine to the brain. Interestingly, a person hasn’t yet experienced any pain. It is not until the signal from the nerve reaches the brain where it is processed and then you may have a response to what just happened.
Experiencing Pain
Your response and experience of the pain is based upon:
- the information taken in from your senses
- information from past experiences that may have been similar
- your current mood
- level of stress at the time
- perception of the situation
All of this is factored into the equation, without you consciously being aware that the brain is processing all this information, and then you decide the degree to which you experience pain. Within milliseconds, the brain decides whether a response to the situation is necessary. In this case, a person might jerk their foot back, scream, sit down, or do another activity in response to what they are experiencing.
However, the brain might not register the pain at all. Take for instance someone who has a severe case of diabetes and who experiences nerve damage in their foot. A bowling ball may fall on their toe or they may step on a nail and not feel the pain at all. This happens because the nerve that would normally send the signal of pain up to the brain has been impaired.
How to Respond to Pain
Depending upon your pain assessment; the type, location, and severity of your pain, you may want to respond to pain appropriately. There are some important tips to remember when it comes to experiencing pain in the body:
- Don’t ignore pain. Pain that is unknown to you or the result of an injury or disease should be assessed by a healthcare provider.
- Avoid painful movement. While your pain is still acute, it may be best to refrain from movement that causes more harm.
- Keep a pain diary. If you continue to experience pain and you’ve already consulted with a doctor or other healthcare provider, keep track of when, where, and how you experience pain. This can help build awareness around your pain.
- Take care of yourself. Be sure to eat well, get good sleep, and exercise (if you can) in order to keep your body healthy. This can help minimize your experience of pain.
- Drink plenty of water. It’s also important to keep the body hydrated.
- Be curious about your pain. Sometimes pain is not what you think. For example, pain in your neck and shoulders may have more to do with a misalignment in your hip. Again, talk to a healthcare professional if you suspect pain may be linked to something else.
- Reduce the amount of stress in your life. Experiencing pain is already a stressful experience. To help keep stress levels low, eliminate other sources of stress in your life as best you can.
These are general suggestions to keep the body healthy while facing pain. There are a great number of causes of pain. So, be sure to consult your doctor or a healthcare professional for suggestions to assist you in your unique situation.
When you do talk to a pain doctor or a healthcare professional, be sure to use the LOCATES pain assessment tool (or another pain assessment scale) to provide the most detail about your experience of pain. This can assist with getting the right treatment and professional support.
Responses to Lower Back Pain Is Changing

Back pain is one of the most common reasons for seeking medical care in the United States. According to the NPR-Truven Health Analytics Health Poll, people are responding to their lower back pain differently than in the past, and their choices seem to vary depending on their education and income levels.
The Survey on Back Pain
On a regular basis, the TruvenHealth Analytics-NPR Health Poll surveys roughly 3,000 Americans to get their opinions on various health topics. During the first half of March 2017, 3002 participants were questioned on their experiences with lower back pain and their responses to it.
Roughly half of the participants (51%) reported that they suffered from lower back pain in the past 12 months. Of these, 58% sought medical care, while 55% said that they found a way to treat the pain themselves, that is, without going to a doctor. Since back pain, in many cases, can get better on its own, it would make sense that some individuals can skip seeing their physician. Furthermore, over-the-counter medication does provide some relief for back pain.
Here are additional results of the study:
- 69% of those who treated the back pain themselves used over-the-counter pain medication; 21% reported using exercise or physical therapy; 18% said they used heat to manage their lower back pain; 17% used rest; and 12% used prescription pain medication.
- Of those that sought medical care, 70% went to a doctor, 14% went to a chiropractor, 4% went to a nurse practitioner, and 3% went to an alternative medicine practitioner.
- Of those who went to a medical professional, 40% were given prescription pain medication, 31% were told to exercise, 20% were given injections, 17% were told to get a massage, 17% were given steroids, 13% were recommended to take over-the-counter medication, and 12% were recommended to have surgery.
- Among the 51% who reported experiencing back pain in the last 12 months, 45% reported that their back pain got better, 25% said that it remained about the same, 25% said that it went away completely, and 5% said that it got worse.
What’s interesting about this survey is that the responses to lower back pain varied depending upon age and annual income. For instance, young adults were the least likely to go to a doctor for back pain; 64% of them reported that they treated the pain themselves.
There were also apparent correlations between income level and a person’s experience of low back pain. For instance, those with an annual income over $50,000 were more likely to say that their pain went away completely. A correlation was also found between education level and level of back pain: those who hadn’t graduated from college were more likely to report a continued problem with lower back pain. It’s important to keep in mind that these correlations need more research, especially exploring some of the contributing factors. For instance, those with a lower level of education might not have access to adequate medical care and have less disposable income to spend on complementary treatments such as acupuncture or massage.
For more information on the relationships between income, education, and reported experiences of back pain, read the survey’s full report.
Lower Back Pain May Not Require Opioids
Every person’s experience of pain is different. Yet, with lower back pain, many people may find that the aches and discomfort will go away on its own with time. Of course, each person’s level of pain and circumstances are different so it’s best to consult with a doctor. However, for those who are have sedentary jobs, do little exercise, experience a great deal of stress, and/or who are overweight, reducing back pain may simply be a matter of making changes to one’s lifestyle. Organizations such as the Center for Disease Control and Prevention (CDC) and the American College of Physicians (ACP) are recommending that individuals try other resources first before asking for a prescription for pain medication. For instance:
- In March of 2016, the CDC issued guidelines recommending that opioids not be the first choice for managing chronic back pain.
- In April of 2017, the ACP published clinical guidelines for managing chronic pain, in which they recommended non-pharmaceutical remedies first such as a heating pad, then over-the-counter medication, and then, if needed, prescription pain pills, beginning with NSAID’s (nonsteroidal anti-inflammatory drugs) first.
The explosive reliance on opioids over the past 15 years to manage pain has in some ways conditioned the American public that they simply need to take a pill to eliminate their pain. Fortunately, with education and growing awareness about the dangers of opioids, more and more people are making better choices, and finding their own ways to manage pain. In fact, in some cases, going to a doctor may be more risky especially if that doctor still endorses the use of opioids as a primary means of relieving pain.
Options for relieving back pain include:
- Exercise (especially the muscles in your core)
- Stretch your hamstrings twice daily
- Change your diet to include healthy foods
- Get the right amount of sleep
- Massage, yoga, or other practices that can reduce stress in the body
- Heating pads
- Over-the-counter medications
- Maintain a healthy weight
- See a chiropractor, physical therapist, or another type of body therapist
- Practice yoga
- Use herbs and supplements
- Practice aquatic therapy or use a jacuzzi regularly
- Try a transcutaneous electrical nerve stimulator (TENS) machine
- Participate in activities that you enjoy
Of course, keep in mind that the above list is simply to provide options. However, these tips may not work for everyone. To get a sense of whether any of the above suggestions may be effective for your condition, speak to a health professional. The point is that there are other methods to help relieve pain without taking prescription drugs. It may be important for anyone who experiences chronic lower back pain to assess their options, discuss those options with a health professional they trust, and develop a plan for living a healthy and pain-free life.
How to Stay Optimistic with Chronic Illness

Chronic illness is a fact of life for about half of American adults, a statistic that has been steadily and tragically growing over the past few decades. It isn’t just poor health and trouble coping with any number of crippling symptoms. It’s also a deep mental anguish that too often transforms from a feeling to a disorder.
Illness and pain come in many shapes and sizes. Some are far more common than others, such as type-I diabetes and arthritis. Others are less common, such as inflammatory bowel diseases or chronic fatigue syndrome. Yet they all share the fact that they’re debilitating, to the point where leading a life of optimism with such a diagnosis shackled to one’s legs can seem like a pipedream.
Yet many make it happen anyway. Not out of sheer bullheadedness, but out of a love for life perpetuated through gratitude and unhindered by bouts of pain and struggle. It’s not just possible to stay optimistic and happy while struggling with a chronic illness – it is necessary if you want to successfully live with the diagnosis.
Acknowledging the Pain of Chronic Illness
We’re not here to make light of anybody’s situation when we say that it’s important to look on the bright side of things when struggling with a chronic illness. We know exactly how terrible they can be, and just how much life and happiness they soak up and raze to the ground.
The definition of a chronic illness is that it is a long-term disease that can last years or even indefinitely, and progressively become harder to combat. These diseases often leave people with disabilities, or secondary conditions including chronic pain. For those who are diagnosed with one, living with it will be their greatest challenge. Like great big wall, it can encompass your entire field of vision. It can hog every detail of your life, and separate you from what could be a great life.
Not all chronic illnesses start out with the same severity, or share that severity from case to case. However, their progressive nature and tendency to last for years or even decades means anyone struck with the diagnosis of a chronic illness will be struggling immensely. Yet in every case, optimism plays a vital role.
Why Optimism Makes a Difference
Chronic illnesses aren’t just a simple diagnosis, like many other diseases. They are notorious for the fact that they’re hard to treat, and can sometimes be untreatable altogether. A chronic condition instead must be managed, and – this is key – lived with.
When confronting something like kidney failure or an open wound, modern medicine can spring to action to ease suffering, kill the pain, and heal the patient. But we can’t just erase chronic illnesses or prevent them through vaccines. All we can do is help ease the long-term suffering of a patient and advise them on the best way to live through life as unhindered as possible.
It’s not rational to hold out for hope that your condition will receive a miracle cure. This sudden sentencing of being given a crippling disease with no guarantee of recovery and no rhyme or reason, can drive people over the edge and off a cliff into the realms of depression and anxiety.
In many ways, it’s not just that the illness itself makes it hard to live a happy life. Our outlook, and our perspective on life makes it hard to live a happy life. That’s why it’s so critical to find optimism, because without it, there’s no hope of “beating” the illness, and of living life to whatever its fullest potential may be in your case.
Then again, a lot of “hot air” and pleasant words won’t do you much good against the reality that you’re stuck finding a way to be happy and grateful while struggling with a long-term illness you didn’t deserve. But there are many ways to cultivate that gratitude, and move on from a life of pessimism and anger to a life of joy.
Boosting Positivity While Ill
First, optimism isn’t about rejecting reality. It’s not about going against nature with force and stubbornness. It’s about rationally realizing the facts of your current limitations, and still finding a way to enjoy yourself and be happy despite them. Chronic illnesses don’t just weaken you physically, they wage war on you mentally. You must fight back by first accepting your new reality, rather than being consumed by anger and sadness over it.
That’s the first step, and it’s the hardest. From there, it’s a matter of improving – and celebrating each improvement – while doing your best to find new ways to circumvent your limitations and still find enjoyment in life, wherever you can find it.
Therapy is important here, not just mentally, but physically. While many chronic illnesses are progressive, you can – with slow and steady therapy – make gains in quality of life. Some illnesses possess a chance of slow recovery through surgery, while others have symptoms are manageable through medication. For every bit of mobility and change, celebrate. And for every setback, remember that it’s fine to be sad and angry – for a time. Huddle up, do something you can do and love doing, and surround yourself with people who can help cheer you up. Focus on the positivity you might have experienced elsewhere in life.
Even the “small” things matter. Being able to walk up a flight of stairs, leave the house, carry some groceries, make some tea, walk your pet. Whatever it is, it doesn’t matter if other people consider it normal. To you, it may be an improvement – and that’s something to be grateful for.
Inspire and Be Inspired
When you can stand up and face your illness with the tenacity and courage to deny it of all the negativity it usually brings, you’re a hero. Not just to yourself, for saving yourself from the pain of constantly bearing that unnecessary emotional weight on your back, but others, for making it clear to them that it’s okay to be sick and happy. In fact, it’s important.
Heroes don’t wear capes. They don’t lift entire buildings or leap from rooftop to rooftop – heroes are saviors. They meddle in people’s lives by becoming a positive influence, a paragon of positivity. Heroes are people who can prove that the odds don’t mean anything when you have human spirit.
You won’t be able to inspire everyone to look on the brighter side of things. Not everyone will see benefits to focusing on the silver lining of their great dark storm – but that doesn’t mean it isn’t worth it.
Most people sadly can’t hold out for a cure to their illness, and may constantly be in pain. Either it hasn’t been developed yet, or the treatment is outside their price range. The reality for millions of Americans is that they must learn to live with their illness. No one wants to. But being able to do so – and still enjoy life, making the most of every moment – takes a lot of strength. It will help others see past the pain and towards the potentially brighter days.
Natural Pain Relievers and Anti-Inflammatories
Medication is not the only reliable way to relieve pain – and for many, long-term medication is not a very suitable way to relieve chronic pain, which can plague a person for years. While most of our pharmaceutical options rely on natural extracts anyway, there are specific benefits towards applying some of nature’s own natural pain relievers in their original form.
But to understand why the common advice of ginger, turmeric, and less known relievers such as cloves all work in the face of specific forms of pain, it’s important to cover the basics of chronic pain, and the common cofactor of physical inflammation in the human body.
Chronic Pain and Inflammation
Chronic pain is a condition wherein a person experiences the sensation of pain regularly for over twelve weeks. Pain experienced regularly within that period is most likely acute. This pain is a derivative of a specific wound or injury, and fading as per the body’s own natural healing.
But our bodies are far from perfect. Through a range of possibilities from nerve damage, to inflammation and psychological illness, the body can achieve a state of chronic pain. Permanently treating chronic pain isn’t always possible, depending on its origins. The primary focus for medicine and treatment is to first look towards effective, long-term relief, while trying to identify the cause and an ultimate solution.
That’s where the science of pain management is most significant. Chronic pain management is a very broad school of knowledge, but its roots lie in understanding how pain travels from the body to the brain and back, and how specific pain relievers can block or counteract the signals.
Types of Inflammation
Inflammation isn’t always directly related to chronic pain, but it’s most definitely a part of pain in general. Inflammation is most often seen in the form of arthritis, a widespread joint inflammation that causes chronic joint pain. It occurs when an injury, infection, or other type of physical irritation or sickness causes the body to heat up and increase the overall sensitivity of a specific part. An inflammation around a wound is typically a sign of infection, for example. As the body’s immune system is working hard to fight foreign bacteria through white blood cells, the increased activity results in heating up the wound, and making it more sensitive to discourage any contact.
If you cut yourself or break a bone, then any attempts to touch the injured area will result in extreme discomfort. Even with a mild or soft touch will hurt, to prevent further damage – the same thing happens in an inflammation.
The problem when inflammation is tied to chronic pain, is that the inflammation may not go away. Aside from the obvious drawback of near-constant pain, an inflammation anywhere in the body will weaken you tremendously, and sap your energy.
In many cases of chronic pain, fighting not just the pain but specifically fighting to lower any internal inflammation often works to further decrease pain. When it comes to natural pain relievers and anti-inflammation, the options for application remain the same: external, and internal.
Topical Natural Pain Relievers
Pain relief often comes in the form of creams and ointments. There are several naturally-derived ointments that are perfect for quick pain-relief, especially in cases of back pain and arthritis. A few examples include:
Among these three Cs, camphor is most often found in ointments and paired with menthol. Capsaicin is the active element in hot peppers. It’s unique nerve interaction causes it to become an effective numbing agent when used right. Comfrey shouldn’t be ingested, but is an active ingredient in a topical cream it is effective for pain management.
Pain Relief Through the Diet
Let food by thy medicine – and despite thousands of years of progress in the sciences, Hippocrates early wisdom still holds true. While a good diet won’t exactly patch up a knife wound or splint a broken arm, most preventative diseases can be greatly diminished and even avoided entirely through healthy lifestyle choices. Genetics, environmental factors such as pollution and even psychological factors can still skew the outcome against you. However, healthy food can keep you fit – or in this case, relieve a lot of pain.
Foods That Lower Inflammation
There are quite a few ways to relieve pain and lower inflammation through food, including:
- Willow bark tea
- Turmeric
- Omega-3 and omega-6 foods
- Other fats
- Leafy greens
- Berries and citrus fruits
Willow bark and turmeric are ancient natural pain relievers, and modern-day aspirin specifically derives from willows. Omega-3 fats are present in seed oils and most plants, while omega-6 fats are in seafood. The trick is doing your best to maintain a low ratio of the two. Research shows that doing this greatly decreases inflammation – rather than just eat more fish, cut down on all seed oils.
Healthy fats come in many shapes and forms. Avocados, coconut, lean meat, fish, and olives are great sources of fat, while seed-derived oils, lard and margarine aren’t. A healthy balance of green vegetables and various fruits also decreases inflammation. Although the jury is still out on exactly why this is, as antioxidants may not be as important as we’ve thought.
Foods to Avoid
Sometimes, what you don’t eat matters as well. There are specific foods to avoid when you’d like to decrease your pain and inflammation, and stay healthier in general. These include:
- Refined sugars/carbs (including white bread and pasta)
- Canned and/or processed meats
- Trans fats, margarine, shortening
- Fried foods (excessive seed oils)
Acupuncture
Other natural pain relievers to consider are a bit more exotic, but shows a kind of promise that is not to be ignored. Acupuncture, an ancient medical practice, is surprisingly effective in many cases of chronic pain although we can’t really say why. The answer might lie in future research, or in the simple placebo effect. Either way, it’s a type of therapy that, considering the odds, would be well worth a shot.
It’s possible that just like acupuncture, some of these topical or natural pain relievers won’t function well. We humans do have a shared biology, but we’re still individually unique – certain factors from genetics to diet and medical history may mean that some tools are far less effective than others. It all depends on the origin and kind of chronic pain being experienced, as well. In terms of anti-inflammation, however, it’s more straightforward and generally applicable. Diet is an effective way of controlling your body’s inflammation, and with time, a good diet and regular exercise can help you lead an enjoyable and fulfilling life even with the diagnosis of chronic pain.
How Fibromyalgia Pain Relates to Other Pain Conditions
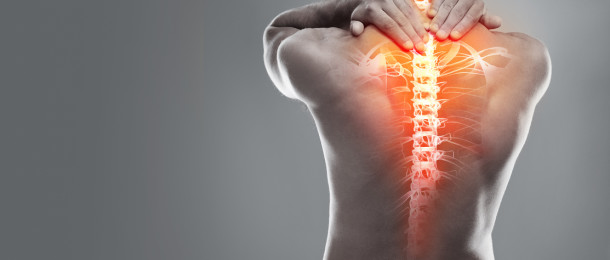
Pain is not something we’re particularly inclined to like, as its intended function is to be something we actively avoid and work against. But there is such a thing as useful pain. Pain that teaches us valuable lessons in life, like avoiding fire and minding our step.
But there is some pain that has absolutely no use, and no meaning. Medically, that pain is part of a series of disorders – conditions like fibromyalgia, which plagues roughly 5 million American adults. These people must live with chronic fatigue, constant soreness, and the combined blight of widespread pain and a heightened awareness towards it. We don’t know what causes this disease. We don’t know what cures it. But we have learned to help people deal with it, and live meaningful lives.
To properly understand this affliction, it’s important to first tackle how pain itself works – and why fibromyalgia is a massive physical ailment with system-wide consequences. We must first understand how fibromyalgia pain relates to other pain conditions before we can understand how to relieve this pain.
What It Means To Be In Pain
The human body processes stimuli and undergoes a series of brain functions to classify the experience and determine how to react to it. When you experience something pleasant, like a hug from someone you care about, your body interprets it accordingly by releasing certain neurochemicals that make us “feel” a certain way. It gets more complicated than that when you enter the realm of psychology and personality, but from a neurological perspective, it’s a mechanical process.
When the body experiences harmful stimuli, the brain receives a different kind of signal, one that lets it know that there’s a potential danger nearby. Before you can even think about contextualizing the pain, the body and your brain react instantly with irritation, or fear, or a reflexive action such as backing away or flinching. In some cases, pain activates our inner fight or flight response, and the release of adrenaline, epinephrine, and norepinephrine.
From an evolutionary standpoint, certain things make us feel pain so we can learn to avoid them. This ranges from something as obviously dangerous and malicious as a powerful smack to the head to something as unexpected as social rejection. When we feel pain, our initial reaction is not to like it, and then we can act on that info. Simple, and effective.
It gets more complicated on a person-to-person basis, though. Pain is generally objective, but the individual experience is subjective. What you consider painful will be different from what your spouse may consider painful, and tolerance levels for pain change from person to person. We also experience pain differently depending on our mood and emotional stability, our psychological state, our expectations of incoming pain, and quite significantly, the various experiences we might’ve had with pain in the past. Generally-speaking, pain can be split between “physical” pain (nociceptive), generated by a cut, a bruise, a broken bone or another injury; neuropathic pain, which isn’t generated by damage to the body but instead direct interaction with the nerves (nerve damage, spinal cord damage, pain disorders); and psychogenic pain, which is a feeling applied to existing pain by deep psychological troubles and worsening expectations.
While pain is meant to be our cautionary friend in most cases, there are times when it’s not quite so effective at doing its job of keeping us safe and healthy. In this case, the body and pain have a long-term toxic relationship, rather than the ideal distant acquaintance.
On Fibromyalgia Pain
Fibromyalgia pain is a full-body affliction that primarily affects your muscles and connective tissue, and the main symptom reported by those suffering from the condition is widespread chronic (more than 12 weeks) pain. In addition, fibromyalgia pain comes with weakness, nerve pain, muscle spasms and twitching, sleep disturbance and fatigue, and a heightened reaction to physical contact and touch (more pain).
While it affects the muscles and connective tissue, fibromyalgia is a disease of the brain. No one knows concretely what causes it other than an individual and subjective combination of genetics and environmental (lifestyle) factors, and there is no direct cure for the disease either. What basically happens when it develops is that your nervous system malfunctions and begins to sense pain when really there shouldn’t be any, and any painful stimuli are made much more powerfully repellent.
This is a neurological disorder, rather than a psychiatric one, and it’s a disorder with such capacity for widespread emotional damage that dealing with it can be an absolute nightmare.
Fibromyalgia is at its core a problem with pain reception, but it’s also very often part of a comorbidity: the combination of different related afflictions. For example, the chronic pain from fibromyalgia can cause chronic headaches, myofascial pain syndrome (constant muscle soreness), and other forms of rheumatoid pain including arthritis in the joints. Like a multiplier, any acute pain or syndrome you’re suffering from is felt more intensely under fibromyalgia pain. A few common comorbidities for fibromyalgia include:
- Chronic fatigue
- Inflammatory bowel disease
- Interstitial cystitis
- Temporomandibular joint dysfunction
- Arthritis
These are forms of inflammation physical irritation, heightening the body’s sense of pain. This is factored in by the body on top of any subjective thoughts, attitudes and experiences you may already have regarding pain – the result is a chronic condition that can affect you either in a localized fashion (severe hip or shoulder pain, or a specific muscle soreness) or in a general fashion.
Dulling the Hurt
As mentioned previously, there is no direct cure for fibromyalgia pain currently available, but there are several non-steroidal and corticosteroid painkillers available per prescription and over-the-counter to combat the chronic pain brought along by fibromyalgia.
Like so many other pain conditions, the danger with this one is that constant pain is bound to complicate the emotional and psychiatric health of many patients, which only further deepens the possible pain and encourages the use of maladaptive coping strategies like addiction and reckless behavior to take the edge off.
Aside from medication, what seems to work best is a lifestyle change. The inflammatory symptoms and increased pain can be managed properly by following a strictly healthy living regimen, including:
- A diet of fresh food, especially nutrient-rich vegetables and fresh seafood.
- Regular albeit moderate exercise, to improve the body’s neurochemical balance and stave off muscle weakness.
- Consistent and long sleep, to ensure as much rest as possible.
- Movement therapies like tai chi and yoga to raise awareness and body control, useful for mentally dulling out the pain.
Every case is different, and every proposed pain management plan must be catered to the patient’s means, symptoms, and total diagnosis. While fibromyalgia isn’t curable, it is highly treatable and manageable, and a lot of people live with it without medication, relying simply on physical and psychological therapy to overcome the pain. Some rely on alternative treatments like acupuncture and cupping therapy. Like chronic pain in general, it’s a long and tough road – but it’s most definitely a life worth living.
Is There a Link Between Weather and Pain?

Pain is that uncomfortable feeling in one or more parts of your body that is seeking attention. It is the body’s way of telling you something is not right and to seek help to resolve the pain. Some examples of pain include migraines, pinched nerves, broken bones, ear aches, pulled muscles, toothaches, and stomach aches. Other types of pain can come from surgery or surgical procedures. Pain also includes chronic pain, back pain or even fibromyalgia.
Pain has been reported by many to become worse when the temperature changes, but is there actually a link between weather and pain?
Pain and Temperature Connections
Many people suffering from pain will tell you they feel worse when a rain is headed their way. Some may say their arthritis flares up when a barometric pressure change approaches. Others may claim to notice differences in pain when the temperature is hot or cold. Everyone has that family member who swears their knee pain predicts stormy weather. And they are usually right in their predictions.
The link between weather and pain is debated among professionals. There are a few scientific studies to support a relationship between pain and temperature changes. If you ask people dealing with pain and temperature changes, however, they will tell you that they do notice a difference. Their joints may ache more when the temperature gets colder, or warmer, or when humidity is high. It’s the opinion of those suffering from pain that matters the most.
Knowing the various types of pain and how different temperatures can affect the body’s pain is an important first step. This knowledge can help you implement sound tips to control the aches and pains that may be associated with weather conditions.
The diverse types of pain are identified by the length of time they have existed. Once your type of pain is identified, you can begin to manage the pain you have.
Types of Pain
Three main types of pain include somatic, visceral and neuropathic. All three of these can be diagnosed as acute pain or chronic pain. Acute pain usually only lasts a few months and happens when soft tissue is damaged. An example may be a sprained wrist or minor cut or burn. Acute pain is less likely to need pain management and most likely will not be affected by weather changes. Chronic pain, on the other hand, lasts much longer than just a few months. It can last years, even without being able to identify the source of pain. Those with chronic pain can feel the severe effects that cold and hot temperatures have on the body.
Managing pain when the temperature changes is a problem faced by many. There are meaningful tips you can implement based on which temperature affects your pain the most.
Cold Temperatures
Chilly weather causes pain for many people with chronic pain, whether that pain is in their joints or back or other parts of the body. When the weather gets colder, inflamed tissues in your body can swell. Because nerves and muscles are sensitive to colder weather, they can create an uncomfortable feeling in the body. Muscles can become tense when the temperature outside gets colder and this too will make your nerves feel pain.
A 2007 study at Tufts University found that those with arthritis felt more and more pain with every 10 degrees drop in temperature. The colder they were, the worse their pain. Unfortunately, this is similar to those who face increased pain when hot temperatures arrive.
Hot Temperatures
The heat and humidity can also create a great deal of discomfort for those suffering from joint or back pain. This may be due to the hot weather increasing inflammation in the body or because it is difficult for some to regulate internal temperatures during weather changes.
Our bodies have set a natural threshold of pain that we can tolerate. When there is a temperature that is out of your “ordinary” zones of tolerance, the brain interprets this as painful. This pain surfaces as joint pain, back pain, headaches, sinus pains and many other internal and external discomforts.
Whether your pain is increased with cold or hot temperatures, there are many ways you can manage your pain during weather changes.
Pain Management Tips for Warmer Temperatures
When it starts getting hot outside, make sure your body is balanced with cooling activities such as sitting in a room that has air conditioning. You can also keep a cool towel around the body parts that are feeling pain. Engage in activities that ease your pain. These can include massage, acupuncture or even stretching. You do not want to participate in activities that put strain on your body. Don’t try to run a marathon in sweltering heat if you have a knee or joint pains. Instead, go swimming or join a water aerobics class.
Drinking a lot of water is a terrific way to help your body regulate its own internal temperatures. Some doctors recommend the “r.i.c.e.” plan. This includes resting, putting ice on the painful area, compression on the area and elevating the area. They also say to keep active because joints can stiffen quickly. Keeping active does not mean overdoing it. Listen to your body as to how much you can participate in activities and when your body says stop, you should stop and rest.
Pain Management Tips for Colder Weather
Keep moving may be the last thing you want to hear when you are feeling pain due to wintry weather changes. However, keeping the joints active will help them stay loose and not stiff. Another tip to manage pain in the winter months is to eat a healthy diet. You can also take a supplement such as vitamin D, which is associated with improving mood levels which are often depressed during winter months. Depression is associated with achy bones and muscles so doing whatever you can to avoid depression is essential.
Other ways to manage pain in colder weather include taking long, hot baths each day. Also dress in warm clothing. Some reports show that wearing wool clothing and using wool blankets to sleep in have decreased pain in those with fibromyalgia.
Whether you are dealing with pain flare ups from hot weather or cold weather, there are several techniques you can implement to ease your pain. The most important thing you can do is discuss your pain with your doctor, who will be able to offer you techniques as well as some medicinal methods you may want to try. By listening to your doctor and to your body, you can learn to manage the way temperature affects your pain and your lifestyle.
When An Injury Turns Into Chronic Pain

Research has shown that pain affects over one hundred million people, as reported by primary care physicians. Addressing pain can be simple for some and extensive for others, depending on the type of injury. You may have a simple fix, like a broken finger that gets a splint and is healed with a few months. Or you may have a pain that can’t be found through any scans, tests or examinations and lasts for years.
Sometimes it can be both. What you think is going to be a quick fix and starts out as an injury turns into chronic pain and a long treatment period. There are many different types of injuries and all of them have the potential to lead to chronic pain if not managed correctly.
Injuries
Acute pain is the pain typically associated with an injury. It is our body’s way of yelling,
“Hey you, there is a problem here. Fix it soon or else.”
Injury is defined as damage, harm or loss, usually from an outside source. There are many types of injuries, just ask any personal injury attorney. I bet you have experienced at least one in your lifetime, if not more. Have you ever sprained your ankle, cut yourself with a knife, or missed the nail and hit your thumb when using a hammer? Then you have had an injury. Ever been in a fender bender and for the two weeks following had a stiff neck? Then you have had an injury.
There are sports related injuries such as pulled muscles, dislocations and shin splints. There are work related injuries that include machine related or toxic substance exposure. There are also construction related injuries, pet related injuries, car related injuries, playground injuries, the list goes on and on. Basically, if you are living your life, you are susceptible to an injury. But that is no reason to stop living. Not at all. Injuries are very fixable and can heal within a short amount of time.
The medical world defines injuries in more specific terms, like soft tissue, bone, skin and by the body part that is injured. Injuries typically last less than 12 weeks. When an injury turns into chronic pain, it can lead to a long treatment period.
How Pain Becomes Chronic
If you are struggling with an injury in which the pain just won’t go away, then you may be experiencing chronic pain. Pain becomes chronic when it does not leave after three or four months. Your three or four months may be feeling more like three or four years. Persistent pain puts a strain on all parts of our lives and can slow us down or stop us altogether.
One study found that your body’s cells can keep a memory of the injury. Even though the injury is healed and gone, the memory of that pain stays with you in the nerves located around the injury. This happens because your nervous system remains sensitive long after the actual injury has healed.
Chronic pain tends to show up more in older adults, but it does not discriminate. It can affect people of all ages. People who have had surgeries, injuries and are obese tend to experience chronic pain more than others. So, just what is chronic pain?
Chronic Pain
Chronic pain is the type of pain that loves to hang around and make your body its home for twelve weeks or more. It’s like that cousin who came for a week’s vacation and is still living with you three months later. It does not go away and it can interfere with your daily routine.
Chronic pain can appear in many different forms. A few examples are headaches, fibromyalgia, back pain, diabetes and arthritis. Sometimes pain can affect you with no diagnosable reason. Over 30 million people are suffering from chronic pain in the United States alone.
The good news, you can get help in managing your pain.
The Importance of Chronic Pain Management
Chronic pain is not something that will just magically disappear and it is not something you should try and manage on your own. A pain management physician is the person you need to help you overcome your pain related issues. He or she has a medical degree and specialized training in pain. They are experts on all things pain. Their goal is to treat your symptoms so you can live a functioning life.
A pain management physician will most likely recommend a variety of treatments and therapies to help you cope with your pain. This is because it is important to treat all areas of your body that will most likely be affected by your pain. The more experts helping you, the better. They will be your own special treatment team and all of them will have the same goal, easing your pain as best they can.
Build Your Team
Your team should consist of a variety of healthcare professionals, friends and family members who truly want to see you succeed in the management of your pain. You do not want people in your life who just want to give you pain pills and let you sleep all day.
A pain management physician is one who can prescribe appropriate medications and monitor you closely to make sure the medicines are working and if not, help you find other medical treatments. They can also examine you on a regular basis and measure for improvements.
A psychologist should be on your team. They can help you work through the mental health issues you may encounter when it comes to pain. They can also help you treat your depression, anxiety or stress that is related to the pain.
A physiatrist and an anesthesiologist are also good team members. A physiatrist has an education in physical medicine and rehabilitation and can treat problems with the brain, nerves, bones, muscles, tendons and more.
A physical therapist can teach you specific exercises and movements that will help you ease pain where it is persistent.
Alternative therapies can also be beneficial to help ease some of your pain. Therapies such as acupuncture, yoga, massages and herbal remedies. There are many holistic practitioners who can help you focus on the mind, spirit, body connection to ease your pain.
Your friends and family should be on your team to help you stay positive, get some exercise, eat healthy and meet other needs your doctors can’t. They are not in your life to enable you, however, only to assist you in completing your own tasks.
Just because you have chronic pain does not mean you can’t have a happy life. There are many resources to assist you in managing your pain. You are valuable, purposeful and worth the effort!
5 Common Causes of Chronic Pain
If you suffer from chronic pain then you know just how devastating it can be to suffer without relief. You know you have a pain, you feel sick, but not one of the many doctors you have seen can identify a source for your pain. It must be very frustrating to know that even the doctors don’t have an answer for you.
After many tests, procedures an examinations, medical professionals have offered you no help and have begun to treat you like you are just making up the pain to continue to receive pain medication. But you would do anything not to need the pain medication or the doctors. There may be a new avenue to try, and it focuses on your mental health, not your medical health. There are different causes of chronic pain, which leads to different types of pain being felt by an individual. We’ll explore the common causes of chronic pain, and how to ease this pain.
Causes of Chronic Pain
The brain is so powerful it can make your body think it has pain. In fact, there are many mental illnesses that actually cause physical pains on a chronic basis.
Mental illnesses such as somatoform disorder, conversion disorder or pain disorder can literally make a person feel pain even though there is no medical cause for the pain. These types of pains can be acute or chronic. Acute pains are temporary and don’t last for very long but they are very noticeable and cause you a lot of discomfort. Chronic pain can last for months or even years without any resolution.
Physical pain can act like a signal, letting us know there is more emotional work to be done. This is why it is so important to address any mental health symptoms that could be causing your chronic pain. Some other mental health disorders that have been shown to produce pain are depression and even post-traumatic stress disorder.
Somatoform Disorder
Somatoform disorder is a mental health illness that makes a person feel chronic pain but there is no physical reason for the pain they are feeling. The diagnostic and statistical manual has defined somatoform disorder as a person having one or more physical complaints but when evaluated medically, no source of the pain can be found. Because of this, people seek medical attention rather than psychiatric care.
Unfortunately, they are rarely helped when they see a medical doctor for this because normally, no medical issue can be found. In addition, patients with this disorder do not believe their problem is psychological mainly because they do actually feel pain. They can’t associate their pain as being a brain problem. When someone feels an actual pain, whether real or not, it is hard to convince them that their pain is really in their mind and not their body.
Conversion Disorder
Conversion disorder is defined as losing the functioning of a physical body part but with no physiological reason for the malfunctioning. These can include paralysis, temporary blindness, loss of smell, or loss of voice.
Conversion disorder usually starts after a traumatic event or psychological conflict. People with personality disorders such as bipolar have proven to experience conversion disorder more times than those without a personality disorder.
Symptoms can last a few days or a few weeks. The best treatment is talk therapy and learning how to cope with stress. Working through your mental health issues with a therapist can help relieve and possibly prevent conversion disorder symptoms.
Pain Disorder
This disorder also deals with the chronic pain felt by a person but the diagnosis is usually related to their psychological problem. Symptoms include feeling helpless about the ability to get relief from pain management, insomnia, fatigue, depression, and anxiety. The person with pain disorder cannot function in a job or in social settings due to their disability.
Sometimes doctors prescribe prescription medications such as opiates to these patients thinking they may have fibromyalgia. However, by the time they realize it is a psychological disorder, the patient is already addicted. Convincing the person they do not need pain medication is nearly impossible due to the brain becoming dependent on the drugs. The brain does not want to quit opiates and it will do what it takes to keep you medicated.
Withdrawal from pain medications is also a hindrance to people quitting their use of the drugs. Furthermore, people who are prescribed pain medications do not necessarily consider themselves addicts because their drugs were given to them by a doctor.
Depression and Chronic Pain
Depression contributes greatly to chronic pain involving arthritis, migraines and backaches. Some reports show that even chest pains and digestive problems can be related to depression. Many people diagnosed with mood disorders complain of physical ailments that have caused them physical and mental disabilities.
Depression can make you feel fatigued and it can be a struggle some days just to get out of bed. A person with severe depression can even become neglectful to their physical health as well as their mental health.
If you are dealing with pain that seems to come around for no reason, take an assessment of your level of depression. You may just find that a very treatable disorder like depression is leading to your physical ailments.
Post-traumatic Stress Disorder and Pain
Post-traumatic stress disorder is an anxiety disorder. It can cause physical pains after a traumatic event. Some examples of post-traumatic stress disorder are fighting in combat during war, sexual abuse as a child or adult, witnessing a murder or even witnessing domestic abuse of a parent.
Post-traumatic stress disorder, if not dealt with in therapy, can start to show itself through physical pain. Suppressed symptoms of post-traumatic stress disorder can be damaging to mental and physical health. These symptoms may include body aches, stomach pains, headaches, and trouble sleeping. One report states that up to 35 percent of people with chronic pain have some form of post-traumatic stress disorder.
Cognitive Behavioral Therapy and Healing
So how do you deal with chronic pain that may be related to a mental illness? Seeing a Psychologist is essential for improvement. A mental health professional can correctly diagnose your disorder and set up a treatment plan to help improve your mental health and ease the physical pains you are feeling. Cognitive behavioral therapy and possibly medication can be a great combination in helping you overcome chronic pain caused by mental health disorders.
Now is the time for you to deal with your pain. You deserve to live pain free and if healing your mental health can get you that life, it is worth every effort. Make today your day to start healing!
Sports Injuries

Recognizing and Preventing Athletic Damages to Your Body
Athletes are some of the fittest individuals in the world. As strong as their bodies are, however, they also can sustain injuries because of the repetitive and stressful motions of their chosen activities. You can stay fit and enjoy your favorite sport or exercise by knowing how to recognize and prevent common sports injuries.
Common Athletic and Exercise-Related Injuries
Any part of your body can become injured while you are playing sports or working out. For instance, your legs, ankles, and even your toes can be injured while you are running or kicking.
Running and kicking invites direct impact to these parts of your body. Whether you are kicking a football or pounding your feet on hard pavement while running, you could suffer from damages like a sprain, strain, or fracture, leaving you unable to compete or work out for weeks or months.
Some activities require that you lift heavy objects. Sports like the discus or shot put, for example, put strain on your arms, shoulders, hands, and upper back. Weightlifting and wrestling can likewise damage your elbows, shoulders, and lower back because of the resistance and duration required for these athletic activities.
When you want to continue your favorite exercises and sports but want to minimize the negative impact they can have on your body, it is important that you know what steps to take to prevent such common injuries. The precautions you take before working out or competing could save you from pain and suffering that could last for weeks, months, or even years.
Preventing and Healing from Sports Injuries
The old adage of an ounce of prevention being worth a pound of cure definitely applies when you exercise or play sports. By preventing sports injuries now, you save yourself the time and distress of healing from them.
Before you engage in your favorite sports or exercises, you should first stretch out to make sure you are limber and warmed up properly. When your body is flexible and ready to go, you prevent damages like strains and sprains to your joints, ligaments, and tendons. You may be encouraged to stretch and warm up a half hour or sooner before playing.
You should wear proper gear when playing your favorite sports. Wearing a helmet while playing football or batting during a baseball game can prevent sports injuries that come from a direct blow to your head. Supportive athletic shoes, gloves, shin guards, and other gear also have a role in keeping your body safe from injuries that could take you out of play for the rest of the season.
If you do suffer from a sports injury, however, it is imperative that you have it professionally diagnosed and treated so that you can heal from it faster. Medical professionals who can diagnose, treat, and monitor your healing can address issues like pain and limited mobility, helping you get back on the court, field, or track quicker.
Playing your favorite sports should be fun and worry-free. When you suffer a sports-related injury, however, your enjoyment may be cut short, forcing you to sit on the sidelines for weeks or longer. You can prolong your play and take care of your body by knowing how to recognize and prevent today’s most common sports injuries.
If you are reading this on any other blog than Comprehensive Pain Management Center or via my RSS Feed, it is stolen content without credit. You can find us on Twitter via @CompPainMgmt. Come and visit our blog at http://www.compainmc.com/blog/.